Trautner, Emily, Kim, Jina, Rabe, Adrian and Thrivikramji, Hari (2021) The cost-effectiveness of immediate vs routine postpartum IUD placement: a UK perspective. Journal of Health Policy and Economics, 1 (1). ISSN 2732-4729
|
Text (Trautner-et-al__IUD-placement-cost-effectiveness--published)
- Published Version
Available under License Creative Commons Attribution. Download (324kB) |
||
![[img]](http://eprints.lse.ac.uk/120040/3.hassmallThumbnailVersion/Figure_4_revised.png)
|
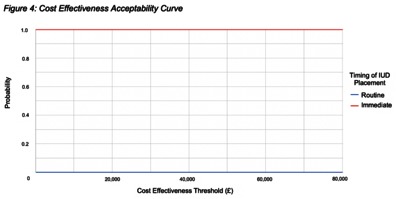
Image (Figure 4_revised)
- Published Version
Available under License Creative Commons Attribution. Download (485kB) | Preview |
|
![[img]](http://eprints.lse.ac.uk/120040/4.hassmallThumbnailVersion/Figure_3.png)
|
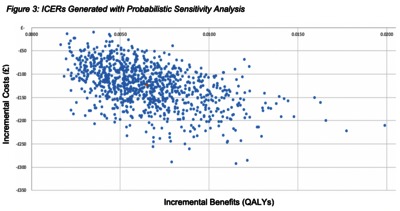
Image (Figure 3)
- Published Version
Available under License Creative Commons Attribution. Download (887kB) | Preview |
|
![[img]](http://eprints.lse.ac.uk/120040/5.hassmallThumbnailVersion/Figure_1_revised.png)
|
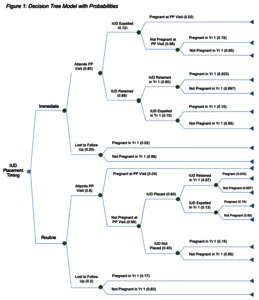
Image (Figure 1_revised)
- Published Version
Available under License Creative Commons Attribution. Download (554kB) | Preview |
|
![[img]](http://eprints.lse.ac.uk/120040/6.hassmallThumbnailVersion/Figure_2.png)
|
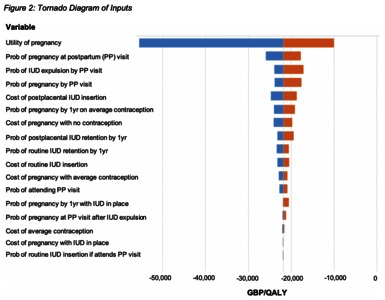
Image (Figure 2)
- Published Version
Available under License Creative Commons Attribution. Download (2MB) | Preview |
Abstract
OBJECTIVES: Preventing pregnancy in the year after childbirth provides health benefits, and an intrauterine device (IUD) placed immediately after birth is a cost-effective tool to prevent pregnancy. However, it is not known if this strategy is cost-effective in the UK context. Therefore, our study objective was to identify the cost-effectiveness of immediate compared to routine IUD placement strategies in the UK. METHODS: A decision tree cost-effectiveness model was constructed using inputs from published literature including data and costs from the National Institute for Clinical Effectiveness (NICE). The study population for this evaluation is women in the UK who desire a postpartum IUD. The perspective of the study was payer and the time horizon was one year. The outcome measure was incremental cost-effectiveness ratio (2018 Great British Pound per quality-adjusted life-year [QALY] gained), with a threshold of an ICER<20,000 considered cost effective. RESULTS: The results of the analysis yielded an ICER of -21,845, which is interpreted as a cost savings of 21,485 GBP for every QALY averted with the immediate placement strategy. Our results and probabilistic sensitivity analysis both indicate that immediate placement is a consistently dominant strategy as compared to routine placement. Results were most sensitive to changes to the health utility assigned to pregnancy. CONCLUSIONS: Immediate as compared to routine postpartum placement of an IUD is a dominant strategy and presents an opportunity for a cost saving policy. Budget impact analysis indicates that savings from the implementation of this strategy over a 5-year time horizon (2019-2023) would be over £17 million.
| Item Type: | Article |
|---|---|
| Official URL: | https://johpec.lse.ac.uk/ |
| Additional Information: | © 2021 The Authors |
| Divisions: | LSE |
| Subjects: | H Social Sciences > HB Economic Theory R Medicine > RA Public aspects of medicine |
| JEL classification: | I - Health, Education, and Welfare > I1 - Health > I10 - General |
| Date Deposited: | 22 Aug 2023 10:06 |
| Last Modified: | 29 May 2025 09:41 |
| URI: | http://eprints.lse.ac.uk/id/eprint/120040 |
Actions (login required)
 |
View Item |

 Download Statistics
Download Statistics Download Statistics
Download Statistics